By Richard Hayes, MD, Great Basin Orthopaedics
Some of us have genetically flat feet without much arch. We may wear arch supports or custom orthotics to improve our comfort when walking. However, there is a difference between a low arch or mildly flattened foot shape and what orthopaedists call acquired flatfoot deformity, or posterior tibial tendon dysfunction (PTTD).
PTTD is one of the most common problems of the foot and ankle I see. It occurs when the posterior tibial tendon becomes inflamed or torn. As a result, the tendon may not be able to provide stability and support for the arch of the foot, resulting in a flattened foot where the entire sole contacts the ground.
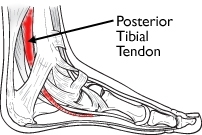
Image from American Academy of Orthopaedic Surgeons
Why do we care if our foot becomes “flat”?
The posterior tibial tendon is one of the most important tendons of the leg. A tendon attaches muscles to bones, and the posterior tibial tendon attaches the calf muscle to the bones on the inside of the foot. The main function of the tendon is to hold up the arch and support the foot when walking.
Without treatment, the flatfoot that develops from posterior tibial tendon dysfunction eventually becomes rigid. Arthritis develops in the hindfoot. Pain increases and spreads to the outer side of the ankle. The way you walk may be affected and wearing shoes may be difficult.
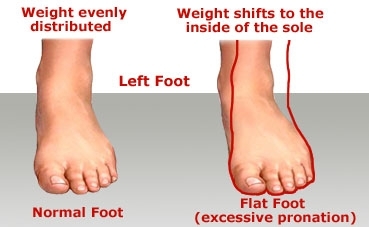
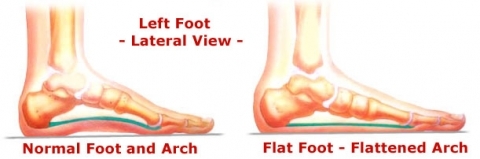
Images from myflatfeet.com
Causes
Overuse of the posterior tibial tendon is often the cause of PTTD. Symptoms often appear after activities that involve the tendon, such as running, walking, hiking, or climbing stairs. People who do high-impact sports, such as basketball, tennis, or soccer, may have tears of the tendon from repetitive use. Once the tendon becomes inflamed or torn, the arch will slowly fall (collapse) over time. An acute injury, such as from a fall, can abruptly tear the posterior tibial tendon or cause it to become inflamed.
Posterior tibial tendon dysfunction is more common in women and in people older than 40 years of age. Additional risk factors include obesity, diabetes, and hypertension.
Signs and Symptoms
Pain and swelling on the inside of the ankle
Loss of the arch and the development of a flatfoot with ankle collapsing in
Gradually developing pain on the outer side of the ankle or foot
Weakness and an inability to stand on the toes
Tenderness over the midfoot, especially when under stress during activity
Nonsurgical Treatment
Many patients can find relief from the symptoms of flatfoot with appropriate nonsurgical treatment. However, it is not uncommon for the pain to last up to 6 months after treatment begins.
Rest: Decreasing or even stopping activities that worsen the pain is the first step. Switching to low-impact exercise is helpful.
Ice: Apply cold packs on the most painful area of the posterior tibial tendon for 20 minutes at a time, 3 or 4 times a day to keep down swelling.
Nonsteroidal Anti-inflammatory Medication: Drugs, such as ibuprofen or naproxen, reduce pain and inflammation. Talk with your primary care doctor if the medication is used for more than 1 month.
Immobilization: A short leg cast or walking boot may be used for 6 to 8 weeks. This allows the tendon to rest and the swelling to go down.
Orthotics: Most people can be helped with orthotics and braces. An orthotic is a shoe insert. It is the most common nonsurgical treatment for a flatfoot.
Braces: A lace-up ankle brace may help mild to moderate flatfoot. The brace would support the joints of the back of the foot and take tension off of the tendon.
Physical Therapy: Physical therapy that strengthens the tendon can help patients with mild to moderate disease of the posterior tibial tendon.
Surgical Treatment
I typically do not consider surgery until the patient has tried 6 months of appropriate non-surgical treatment without significant relief. The type of surgery performed depends on where tendonitis is located and how much the tendon is damaged. Surgical reconstruction can be extremely complex. These are some of the more common operations:
Tenosynovectomy: In this procedure, the surgeon will clean away (debride) and remove (excise) any inflamed tissue surrounding the tendon.
Osteotomy: This procedure changes the alignment of the heel bone (calcaneus). The surgeon may sometimes have to remove a portion of the bone.
Tendon transfer: This procedure uses some fibers from another tendon (the flexor digitorum longus, which helps bend the toes) to repair the damaged posterior tibial tendon.
Lateral column lengthening: In this procedure, the surgeon removes a small wedge-shaped piece of bone from either your hip or that of a cadaver and places it into the outside of the calcaneus. This helps realign the bones and recreates the arch.
Arthrodesis: This procedure welds (fuses) one or more bones together, eliminating movement in the joint. This stabilizes the hindfoot and prevents the condition from progressing further.
The bottom line is don’t ignore a fallen arch or flattening foot. The discomfort will only increase overtime and may become quite debilitating. See a qualified orthopaedist for an evaluation and learn about your treatment option.
Dr. Richard Hayes is a Board Certified orthopedic surgeon at Great Basin Orthopaedics. He is Reno’s first fellowship-trained foot and ankle specialist and received training at the prestigious Campbell Clinic in Memphis, Tennessee. Great Basin Orthopaedics has been providing Northern Nevada with exceptional orthopaedic care since 1964.
Sources:
American Academy of Orthopaedic Surgeons, Posterior Tibial Tendon Dysfunction, http://orthoinfo.aaos.org/topic.cfm?topic=A00166
American Orthopaedic Foot & Ankle Society website, Ailments of the Midfoot, http://tinyurl.com/bqxgztj